By: Rhea Tomlinson (BMR-PT, BA)
Certified in Acupuncture & Dry Needling
RYT 200 hour
What is Acupuncture & Dry Needling? Does it hurt? What are my risks? Are these treatments effective? These are questions we get all of the time in clinic. This blog will help you answer all of these questions and more!
What is Acupuncture?
Acupuncture is a holistic health technique that stems from traditional Chinese Medicine practices in which certified practitioners stimulate specific, pre-mapped out points along lines called meridians on the body. Acupoints are stimulated most commonly by inserting thin, single use, sterile needles into the skin. Acupuncture is said to stimulate endorphin release, circulation surrounding the points for swelling control and healing, and helps to release myofascial (muscle) tension.
In traditional Chinese medicine, acupuncture is linked to the belief that disease is caused by disruptions to the flow of energy, or qi (energy flow) in the body. Acupuncture stimulates points on or under the skin called acupuncture points or acupressure points, unblocking this qi travelling along the meridians. Western scientific research believes acupuncture stimulates neurohormonal pathways. Acupuncture itself doesn’t directly release feel-good chemicals that can aid in inflammation, stress, but it works higher up the chain such as affecting the pituitary gland to produce the extra hormones, or excites the nerves (Palmero, 2017).
What is Dry Needling?
According to Kinetacore (2003) dry needling is a general term for a therapeutic treatment procedure that involves multiple advances of a filament needle into the muscle in the area of the body which produces pain and typically contains a ‘Trigger Point’. There is no injectable solution and typically the needle which is used is very thin. Most patients will not even feel the needle penetrate the skin, but once it has and is advanced into the muscle, the feeling of discomfort can vary drastically from patient to patient. Typically, positive results are apparent within 2-4 treatment sessions but can vary depending on the cause and duration of the symptoms, overall health of the patient, and experience level of the practitioner. Dry needling is an effective treatment for acute and chronic pain, rehabilitation from injury, and even pain and injury prevention, with very few side effects which will be further explained later.
What to Expect During Treatment
Acupuncture and dry needling points are located throughout the body. Sometimes the appropriate points are far removed from the area of pain. The physiotherapist informs the patient about the general site of the planned treatment and if any clothing needs to be removed. If appropriate, a gown, towel or sheet will be provided. The patient then lies on a treatment table in a comfortable position.
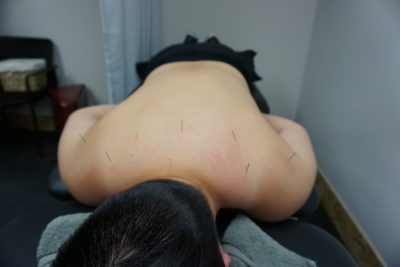
Acupuncture needles are very thin, so insertion creates very little if any discomfort. A mild aching sensation may occur. Typically, acupuncture is very relaxing, and clients will sometimes even fall asleep in a safe position. Acupuncture needles are left in for 15-40 minutes and then discarded in a sharps container to be safely disposed of at a local pharmacy.
According to Kinetacore (2018), for dry needling a healthy muscle produces very little discomfort with insertion of the needle; however, if the muscle is sensitive and shortened or has active trigger points within it, the subject may feel a sensation much like a muscle cramp which is often referred to as a ‘twitch response’. The twitch response has a biochemical characteristic to it which it is believed to improve symptoms in the muscle.
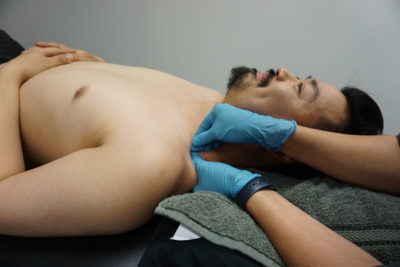
Along with the health of the tissue, the expertise of the practitioner can also attribute to the variation of outcome and/or discomfort. The patient may only feel the cramping sensation locally or they may feel a referral/radiation of pain or similar symptoms for which they are seeking treatment. A reproduction of their pain can be a helpful diagnostic indicator of the cause of the patient’s symptoms. Patients soon learn to recognize and even welcome this sensation as it results in deactivation of the trigger point, thereby reducing pain and restoring normal length and function of the involved muscle (www.kinetacore.com,).
Who should NOT be needled?
If you have the following you should not be needled:
- Pregnancy
- Cancer
- Active infection
- Pacemaker
- Extreme anxiety about being needled
- Consent denied from the patient
- Compromised immune system
If you have the following you should discuss with your practitioner and proceed with caution:
- Allergy to metals
- Bleeding Disorders/on anticoagulants
- Extreme hypersensitivity
- Recent surgery
- Vascular disease
- Cognitive impairment limiting ability for informed consent
What are the risks?
Most of the risks for acupuncture and dry needling are the same.
Vulfsons & Kalichman (2012) summarized several adverse effects associated with dry needling, including post‐needling soreness, hemorrhages (bleeding) at the needling site, syncopal (fainting) responses, and hematoma (severe bruising). Very small risk (<1/10,000) of lung puncture (pneumothorax) or nerve injury (p.410).
The most common risk factor is post needling soreness, mild bruising, or reproduction of symptoms followed by reduction of symptoms.
White & Hayhoe (2001) surveyed 32,000 patient consultations of doctors and physiotherapists who practice acupuncture in the UK. The incidence of adverse events following acupuncture performed by doctors and physiotherapists can be classified as minimal; some avoidable events do occur. Acupuncture seems, in skilled hands, one of the safer forms of medical intervention (p.486).
What is the Research Saying About Needling?
Cummings & White (2001), performed a systemic review of 23 papers on the management of myofascial trigger point pain. They found marked improvements occurred in all groups in which trigger points were directly needled. They believe further research is required to investigate whether trigger point needling has an effect beyond placebo, with emphasis on the use of an adequate control for the needle (www.ncbi.nlm.nih.gov).
Furlan et al. (2005), performed a meta-analysis of 39 randomized controlled trials on the effectiveness of needling, data suggest that acupuncture and dry-needling may be useful adjuncts to other therapies for chronic low back pain. Because most of the studies were of lower methodologic quality, there is a clear need for higher quality trials in this area. Their data suggest that acupuncture and dry-needling may be useful adjuncts to other therapies for chronic low back pain (p.961).
Tough et al., (2009) show in their randomized controlled trial of 39 patients half in a dry needling group and half in a sham group (fake needles) that the dry needling treatment is effective in relieving the pain and in improving the quality of life of patients with myofascial pain syndrome (p.3).
According to Cagnie, et al. (2013) a strong placebo effect was documented, and more large-scale, controlled clinical trials are needed to evaluate the true, unbiased clinical value of this technique (p.345).
Unverzagt et al. (2015) performed a meta-analysis and in summary found that, dry needling research is still in its infancy. However, there is mounting evidence that the procedure can be effective at decreasing pain, improving range of motion, reducing the sensitivity of myofascial trigger points, and ultimately improving quality of life (www.ncbi.nlm.nih.gov/pmc/articles/PMC4458928/).
Take home message:
Different treatments work for different people. Where some people see excellent results with needling, others may experience none at all. Needling has not been proven to be a cure all yet, and more studies are currently needed in the area. To date, needling has shown to be an effective method of pain control, especially for those with myofascial pain syndrome and chronic lower back pain. Needling is very low risk when performed by a competent practitioner and can be a great compliment to your exercise-based physiotherapy or yoga therapy program.
If you have questions about this blog or want to try needling, feel free to contact our amazing Zen Physiotherapy team for more information!
References
Cagnie B, Dewitte V, Barbe T, Timmermans F, Delrue N, Meeus M. (2013). Physiologic effects of dry needling. Current Pain Headache Reports. (17). P.348-356.
Chou, L.W., Kao, M.J., Lin, J.G. (2012). Probable mechanisms of needling therapies for
myofascial pain control. Evidence Based Complement Alternative Medicine. Retrieved May 20, 2018 from www.hindawi.com/journals/ecam/2012/705327/.
Chu, J, Schwartz, I. (2002).The muscle twitch in myofascial pain relief: effects of acupuncture and other needling methods. Electromyography Clinical Neurophysiology. 42(5):307–11.
Cummings, T.M., White, A.R. (2001). Needling therapies in the management of myofascial trigger point pain: A systematic review. Archives of Physical Medicine. (82) p. 986-992.
Furlan, A. D., Van Tulder, M., Cherkin, D., Lao, L,., Koes, B., Berman, B. (2005). Acupuncture and dry needling for low back pain: An updated systematic review within the framework of the cochrane collaboration. Spine 30(8), 944- 963.
Kinetacore. (2018). What is Dry Needling? Retrieved May 20, 2018 from http://www.kinetacore.com/faq/#whatis.
Macpherson, H., Scullion, A., Thomas, K.J., Walters, S. (2004). Patient reports of adverse events associated with acupuncture treatment: a prospective national survey. Quality & Safety in Healthcare, (5) 349-55.
Palmero, E. (2017). What is Acupuncture? Retrieved May 20, 2018 from: https://www.livescience.com/29494-acupuncture.html.
Tekin L, AdarsuS, Durmus O, Cakar E, Dincer U, Kiralp MZ. (2007). The effect of dry needling in the treatment of myofascial pain syndrome: a randomized double-blinded placebo-controlled trial. Clinical Rheumatology, 1-7.
Tough, E.A., White, A.R., Cummings, T.M., Richards, S.H., Campbell, J.L. (2009) Acupuncture and dry needling in the management of myofascial trigger point pain: A systematic review and meta-analysis of randomised controlled trials. European Journal of Pain. (13), 3-10.
Unverzagt, C. Berglund, K., Thomas, J.J. (2015). Dry Needling for Myofascial Trigger Point Pain: A Clinical Commentary. International Journal of Sports Physical Therapy. 10(3) 402–418, retrieved May 20, 2018 from www.ncbi.nlm.nih.gov/pmc/articles/PMC4458928/.
Vulfsons, S. Kalichman, L. Trigger Point Needling: Techniques and Outcome. Current Pain and Headache Reports 16 (5), 407-412.
White, A., Hayhoe, S., Hart, A., Ernst, E. (2001). Adverse events following acupuncture: prospective survey of 32,000 consultations with doctors and physiotherapists. British Medical Journal (323), 485-486.

